Ever heard the phrase there’s nothing wrong with you, the pain is all in your head? Frustrating to hear and seems a very unhelpful thing to say. But is there any basis to this argument? A recent article from the pain researchers at The University of Sydney explain this topic well, they explain it’s not just in your head but in your brain and spinal cord. The recent article, titled How Pain Changes Your Brain, explores the concept of how pain modifies the body and why it sticks around long after the injury has resolved. Their team is looking at exciting new ways to assist the millions of people who live with chronic pain everyday.
Chronic pain affects one in five Australians, young and old. It’s reported to cost the nation $140 billion dollars per year in both treatment and lost productivity. Furthermore, it is estimated that 10-20% of injuries which present to hospital progress to chronic pain conditions.
What happens with chronic pain?
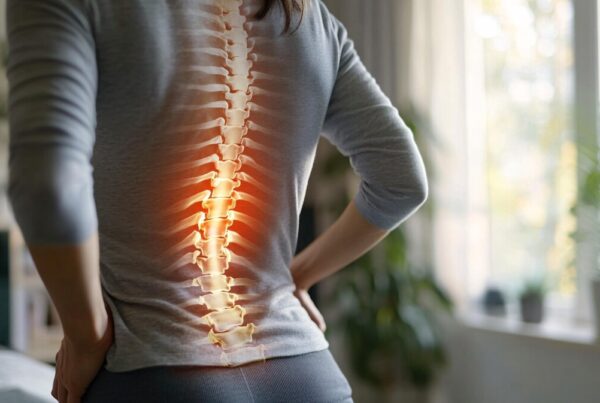
Let’s use the back as an example. Pain is the end result of a sequence of events. The simple story goes a little like this. We start with an injury, like twisting awkwardly while lifting something and hurting our back. This stimulates nearby receptors which detect damage. These receptors send a danger signal along the nerve fibres, or the body’s wiring system. This danger signal reaches the spinal cord, which is a larger network of nerve fibres and a decision is made by neurons in the spinal cord to either do something about it or ignore it. If the danger signal is strong enough or important enough it passes the signal up the next series of nerves to the brain which processes the signal. It is in the brain where the danger signal is computed into pain. This pain is classified by intensity, type and location. The pain also gives us an emotional response and has deep connections with our memory.
Somehow, we can get stimulation of this danger signal process long after the injury has healed. The receptors at the injury site, the nerves that connect these receptors to the brain, or the brain itself can become hyper excitable, or sensitised. It no longer takes an injury to cause our pain but we experience pain regardless. If this doesn’t settle naturally we are left with chronic pain.
What can we do about chronic pain?
The topic is vast and complex. Adaptations in brain cell signalling and our pain experiences mean there is no one size fits all approach. In physiotherapy we recommend a multifaceted approach including activity modification, guidance through movement, exercise and pain relieving treatment.
The researchers in this article are investigating the application of stem cells to target the spinal and brain cells that maladapt to pain. The idea is not to treat pain but to restore the normal signalling pathway.
There are other exciting findings to their research including the interaction of cholesterol medication and pain relief, or the importance of understanding our genetics with pain. A vast and interesting topic, I recommend taking a look at the article linked above.
If you suffer from pain and would like to consult one of our experienced Physiotherapists, please reach out to one of our four Sydney city Bend + Mend clinics.