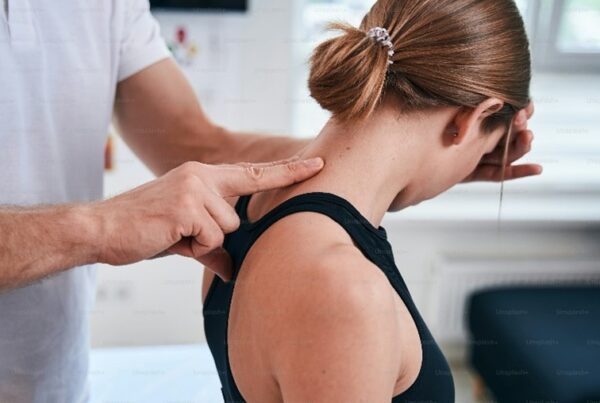
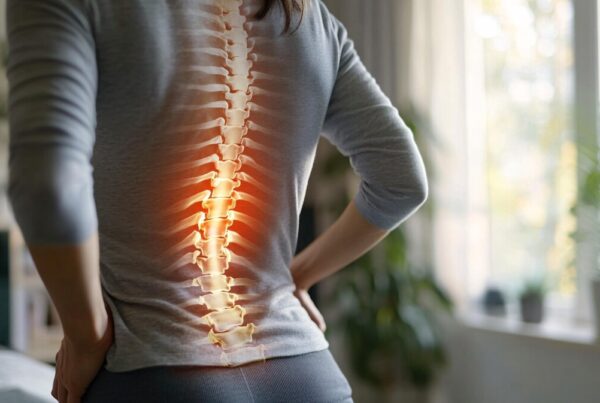
Baker’s cyst, also known as a popliteal cyst, is a fluid-filled sac that forms in the back of the knee. It typically develops because of underlying knee joint conditions, and while it’s usually harmless, it can cause discomfort and limit knee mobility. Understanding the anatomy and underlying causes of Baker’s cyst is crucial for recognizing and managing this condition.
A Baker’s cyst forms in the popliteal fossa, a small, naturally occurring space located behind the knee joint. This cyst is typically filled with synovial fluid, a lubricating substance found in the knee joint.
Causes:
Baker’s cysts often develop as a secondary condition due to underlying knee problems, including:
- Osteoarthritis: The gradual breakdown of cartilage in the knee joint can lead to increased synovial fluid production, contributing to cyst formation.
- Rheumatoid Arthritis: Inflammatory arthritis can cause knee joint inflammation and, subsequently, a Baker’s cyst.
- Meniscal Tears: A tear in the knee’s meniscus (cartilage) can lead to increased synovial fluid production and cyst development.
- Injuries: Direct injuries to the knee joint, such as sprains or trauma, can trigger cyst formation.
Signs and Symptoms:
Common signs and symptoms of Baker’s cyst include:
- Swelling: A noticeable lump or swelling behind the knee, which may change in size.
- Pain: Discomfort or pain in the back of the knee, especially when extending or flexing the leg.
- Stiffness: Reduced range of motion in the knee joint, particularly during activities that involve bending the knee.
Management Strategies:
- Treat Underlying Conditions:
- Addressing the underlying causes of Baker’s cyst, such as osteoarthritis or rheumatoid arthritis, is essential for long-term management. Your physiotherapist can help you to develop a treatment plan tailored to your specific condition.
- Rest and Elevation:
- Resting the affected leg and elevating it above heart level can help reduce swelling and discomfort. Elevate your leg whenever possible, especially after physical activity.
- Ice Therapy:
- Apply a cold compress or ice pack to the cyst for 15-20 minutes at a time, several times a day. This can help alleviate pain and reduce swelling.
- Medications:
- Over-the-counter pain relievers like ibuprofen or prescribed medications may be recommended by a healthcare provider to manage pain and inflammation. Always follow dosage instructions and consult your healthcare provider before starting any medication.
- Physiotherapy:
- Your physiotherapist can design a personalized exercise program to improve knee mobility and strength. These exercises help reduce the cyst’s size and alleviate symptoms.
- Aspiration:
- In some cases, a healthcare provider may perform aspiration, which involves using a needle to drain the cyst. This can provide immediate relief and may be followed by a corticosteroid injection to reduce inflammation.
- Corticosteroid Injections:
- Corticosteroid injections into the cyst can help reduce inflammation and alleviate pain. These injections are often performed in conjunction with aspiration.
- Surgery:
- Surgical removal of the cyst may be considered if it causes significant pain, restricts mobility, or does not respond to other treatments. This procedure, known as cyst excision, involves removing the cyst and addressing any underlying issues.
If you are concerned that you may have a bakers cyst, please contact our team at Bend + Mend to arrange for one of our experienced Physiotherapists to provide you with an assessment.